14 Tech Trends Quietly Transforming Healthcare
Healthcare stands at the precipice of a technological revolution that is fundamentally reshaping how we diagnose, treat, and prevent diseases. While headlines often focus on dramatic breakthroughs, the most profound transformations are occurring quietly behind the scenes, driven by incremental innovations that collectively represent a seismic shift in medical practice. From artificial intelligence algorithms that can detect cancer with superhuman accuracy to nanotechnology that delivers targeted therapies at the cellular level, these emerging technologies are not merely improving existing healthcare paradigms—they are creating entirely new ones. The convergence of computing power, biotechnology, materials science, and data analytics has created an unprecedented opportunity to personalize medicine, democratize access to care, and extend human healthspan in ways previously confined to science fiction. This silent revolution is characterized by its multifaceted nature, touching every aspect of healthcare from prevention and early detection to treatment and recovery, while simultaneously addressing long-standing challenges such as healthcare accessibility, cost containment, and clinical efficiency. Understanding these transformative trends is crucial for healthcare professionals, policymakers, and patients alike, as they collectively represent the future of medicine and the promise of more effective, accessible, and personalized healthcare for all.
1. Artificial Intelligence in Diagnostic Imaging: Seeing Beyond Human Capability

Artificial intelligence has emerged as a game-changing force in diagnostic imaging, revolutionizing how medical professionals interpret complex visual data and detect diseases with unprecedented precision. Advanced machine learning algorithms, particularly deep learning neural networks, are now capable of analyzing medical images—including X-rays, CT scans, MRIs, and mammograms—with accuracy levels that often surpass experienced radiologists. These AI systems excel at identifying subtle patterns and anomalies that might escape human detection, particularly in early-stage diseases where intervention can be most effective. For instance, Google's DeepMind has developed AI models that can detect over 50 eye diseases from optical coherence tomography scans with 94% accuracy, while IBM's Watson for Oncology assists in cancer diagnosis by analyzing vast amounts of medical literature and patient data. The technology's ability to process thousands of images in minutes, rather than hours, is addressing critical radiologist shortages worldwide while reducing diagnostic delays that can be life-threatening. Moreover, AI-powered imaging is democratizing access to expert-level diagnostics in underserved regions where specialist radiologists are scarce, enabling remote diagnosis and telemedicine applications that bring world-class medical expertise to rural and developing areas. As these systems continue to learn from ever-expanding datasets, their diagnostic capabilities are expected to improve exponentially, promising a future where diseases are detected earlier, more accurately, and with greater consistency across all healthcare settings.
2. Wearable Health Monitors: Continuous Surveillance for Preventive Care

The proliferation of sophisticated wearable health monitoring devices is transforming healthcare from a reactive model focused on treating illness to a proactive approach emphasizing prevention and early intervention. Modern wearables have evolved far beyond simple step counters to become comprehensive health surveillance systems capable of monitoring vital signs, detecting irregular heart rhythms, tracking sleep patterns, measuring blood oxygen levels, and even monitoring glucose levels non-invasively. Devices like the Apple Watch have gained FDA approval for electrocardiogram functionality and atrial fibrillation detection, while companies like Fitbit and Garmin continue to expand their health monitoring capabilities with stress tracking, skin temperature monitoring, and advanced sleep analysis. These devices generate continuous streams of physiological data that can reveal subtle changes in health status long before symptoms become apparent, enabling early intervention that can prevent serious complications. The integration of artificial intelligence with wearable technology is creating personalized health insights that can predict potential health issues based on individual baseline patterns and population health data. For chronic disease management, particularly conditions like diabetes, hypertension, and heart disease, continuous monitoring provides both patients and healthcare providers with real-time data that enables more precise treatment adjustments and better adherence to therapeutic regimens. As sensor technology becomes more sophisticated and miniaturized, future wearables promise to monitor an even broader range of biomarkers, potentially including blood chemistry, hydration levels, and inflammatory markers, creating a comprehensive picture of individual health that enables truly personalized preventive care.
3. Telemedicine and Remote Patient Monitoring: Healthcare Without Boundaries

The rapid advancement and adoption of telemedicine technologies have fundamentally altered the landscape of healthcare delivery, breaking down geographical barriers and making quality medical care accessible to patients regardless of their location. This transformation has been accelerated by improvements in high-speed internet connectivity, mobile device capabilities, and cloud-based healthcare platforms that enable secure, real-time communication between patients and healthcare providers. Remote patient monitoring systems now allow healthcare professionals to track patient vital signs, medication adherence, and symptom progression from a distance, reducing the need for frequent in-person visits while maintaining high standards of care. These systems are particularly valuable for managing chronic conditions such as diabetes, hypertension, and heart failure, where continuous monitoring can prevent complications and reduce hospital readmissions. The integration of artificial intelligence with telemedicine platforms is enhancing diagnostic capabilities through symptom checkers, triage systems, and decision support tools that can guide both patients and providers toward appropriate care pathways. Mental health services have been revolutionized through teletherapy platforms that provide access to counseling and psychiatric services in areas where such specialists are scarce, while also reducing the stigma associated with seeking mental health treatment. The COVID-19 pandemic demonstrated the critical importance of telemedicine infrastructure, leading to rapid regulatory changes and reimbursement policies that support remote care delivery. As 5G networks expand and virtual reality technologies mature, the future of telemedicine promises even more immersive and effective remote care experiences, including virtual consultations that closely replicate in-person examinations and remote surgical guidance that brings specialist expertise to any location.
4. Precision Medicine and Genomic Sequencing: Tailoring Treatment to Individual DNA

Precision medicine represents a paradigm shift from the traditional one-size-fits-all approach to healthcare, leveraging advances in genomic sequencing, molecular diagnostics, and data analytics to deliver personalized treatments based on individual genetic profiles, lifestyle factors, and environmental influences. The dramatic reduction in DNA sequencing costs—from billions of dollars for the first human genome to under $1,000 today—has made genomic analysis accessible for routine clinical use, enabling healthcare providers to identify genetic predispositions to diseases, predict drug responses, and select optimal treatment strategies for individual patients. Pharmacogenomics, the study of how genetic variations affect drug metabolism and efficacy, is revolutionizing medication prescribing by identifying which patients are likely to benefit from specific drugs and which may experience adverse reactions. Cancer treatment has been particularly transformed by precision medicine approaches, with tumor sequencing enabling oncologists to identify specific genetic mutations driving cancer growth and select targeted therapies that attack these molecular vulnerabilities while sparing healthy tissue. The development of liquid biopsies, which detect circulating tumor DNA in blood samples, is enabling earlier cancer detection and real-time monitoring of treatment response without invasive tissue sampling. Beyond cancer, precision medicine is advancing treatment for rare genetic diseases, cardiovascular conditions, and psychiatric disorders by identifying the molecular mechanisms underlying these conditions and developing targeted interventions. As artificial intelligence algorithms become more sophisticated at interpreting complex genomic data and predicting treatment outcomes, precision medicine promises to become increasingly precise, potentially enabling the prevention of diseases before they manifest and the development of truly personalized therapeutic regimens that optimize efficacy while minimizing side effects.
5. Robotic Surgery: Precision and Minimally Invasive Procedures
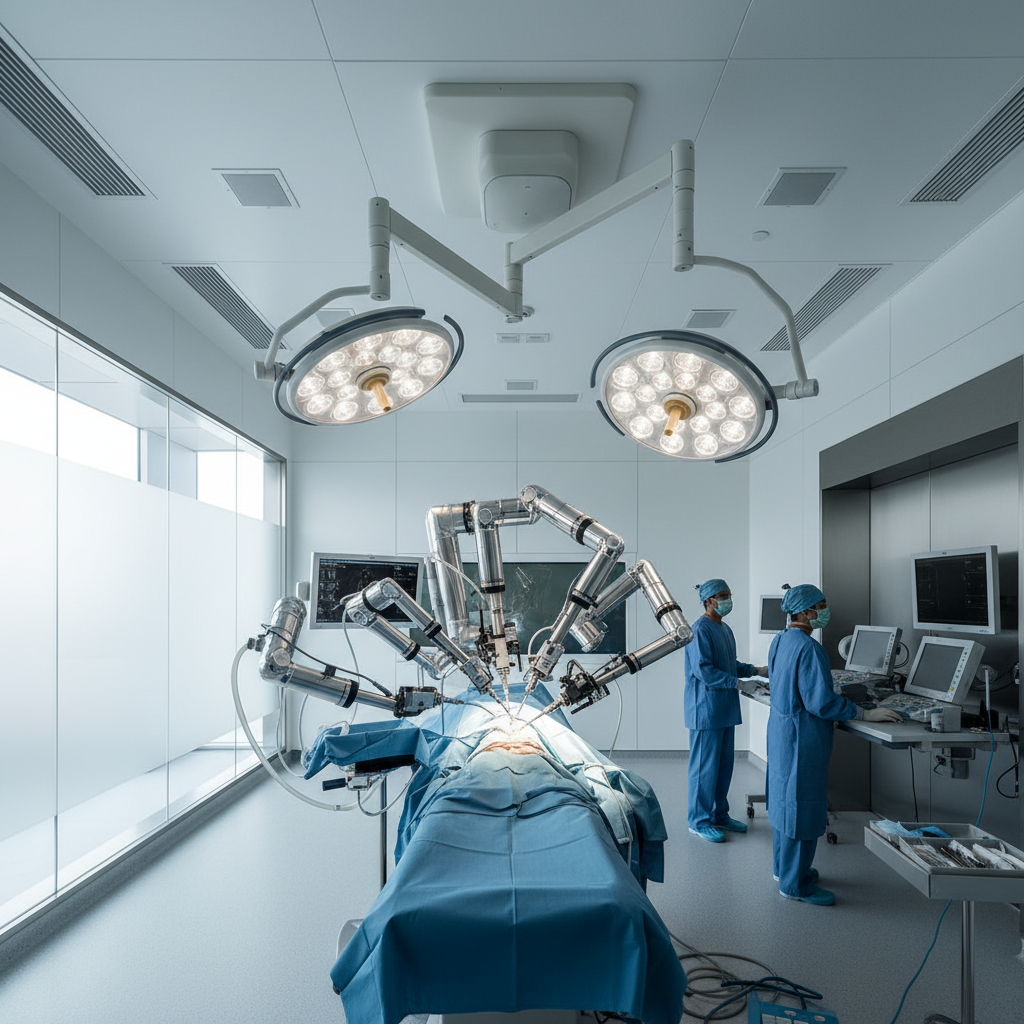
Robotic surgery has evolved from experimental technology to a transformative force in modern surgical practice, offering unprecedented precision, enhanced visualization, and improved patient outcomes through minimally invasive procedures. Advanced robotic surgical systems, such as the da Vinci Surgical System and newer platforms like the Versius and Hugo systems, provide surgeons with enhanced dexterity, tremor elimination, and three-dimensional high-definition visualization that surpasses human capabilities. These systems translate the surgeon's hand movements into precise micro-movements of surgical instruments, enabling complex procedures to be performed through small incisions that result in reduced trauma, faster recovery times, and improved cosmetic outcomes. The integration of artificial intelligence and machine learning into robotic surgical platforms is creating intelligent systems that can assist surgeons in real-time decision-making, provide haptic feedback, and even perform certain routine tasks autonomously under surgeon supervision. Microsurgery, in particular, has been revolutionized by robotic assistance, enabling procedures such as nerve repair, tissue transplantation, and complex reconstructive surgery with precision measured in micrometers. The development of single-port robotic systems is further advancing minimally invasive surgery by enabling complex procedures to be performed through a single small incision, reducing surgical trauma even further. Remote robotic surgery, enabled by 5G networks and advanced telecommunications, promises to bring specialist surgical expertise to underserved areas where such specialists are not available locally. As haptic feedback technology improves and artificial intelligence becomes more sophisticated, future robotic surgical systems may incorporate real-time tissue analysis, predictive complication detection, and automated surgical planning that optimizes outcomes while reducing operative time and surgeon fatigue.
6. 3D Bioprinting: Manufacturing Living Tissues and Organs

Three-dimensional bioprinting represents one of the most revolutionary technologies in regenerative medicine, offering the potential to address the critical shortage of donor organs while advancing personalized medicine through the creation of patient-specific tissues and organs. This cutting-edge technology combines 3D printing techniques with living cells, biomaterials, and growth factors to construct complex biological structures that can function as natural tissues. Current bioprinting capabilities include the creation of skin grafts for burn victims, cartilage for joint repair, and blood vessels for cardiovascular applications, with researchers successfully printing functional tissues that integrate with the patient's existing biological systems. The technology utilizes various bioinks—specialized materials containing living cells—that can be precisely deposited layer by layer to create structures with the complex architecture and cellular organization found in natural tissues. Advances in stem cell research and induced pluripotent stem cell technology are expanding the possibilities for bioprinting by providing sources of patient-specific cells that can differentiate into any tissue type without risk of immune rejection. Pharmaceutical companies are increasingly utilizing bioprinted tissues for drug testing and development, creating more accurate models of human physiology that can better predict drug efficacy and toxicity compared to traditional animal models or cell cultures. The integration of artificial intelligence with bioprinting technology is optimizing printing parameters, predicting tissue behavior, and designing complex structures that maximize functionality and integration with existing tissues. While full organ printing remains a significant challenge due to the complexity of vascular networks and cellular organization required for large organs, recent breakthroughs in vascular bioprinting and organoid technology suggest that printed hearts, kidneys, and livers may become clinical realities within the next decade.
7. Nanotechnology in Drug Delivery: Targeted Therapy at the Molecular Level

Nanotechnology is revolutionizing drug delivery by enabling the precise targeting of therapeutic agents to specific cells, tissues, or organs while minimizing side effects and maximizing therapeutic efficacy. Nanoparticles, typically measuring between 1-100 nanometers, can be engineered to carry drugs, genes, or imaging agents directly to diseased cells while bypassing healthy tissue, representing a fundamental advancement in therapeutic precision. These nanoscale delivery systems can be designed with surface modifications that enable them to recognize and bind to specific cellular targets, such as cancer cells or inflamed tissue, while remaining invisible to the immune system during circulation. Liposomal drug delivery systems, one of the most successful applications of nanotechnology in medicine, encapsulate drugs within lipid-based nanoparticles that can cross biological barriers and release their payload in response to specific environmental triggers such as pH changes or temperature variations. Cancer treatment has been particularly transformed by nanotechnology, with nanoparticle-based chemotherapy drugs showing improved efficacy and reduced toxicity compared to conventional formulations, while gold nanoparticles are being developed for targeted cancer cell destruction through controlled hyperthermia. The development of smart nanoparticles that can respond to multiple stimuli simultaneously is enabling sophisticated drug release profiles that can maintain therapeutic levels over extended periods or deliver multiple drugs in precise sequences. Nanotechnology is also advancing gene therapy by protecting genetic material during delivery and facilitating cellular uptake, potentially enabling treatments for previously incurable genetic diseases. As manufacturing techniques become more sophisticated and our understanding of nano-bio interactions improves, future nanotechnology applications may include programmable nanorobots that can perform complex therapeutic tasks within the body, such as clearing arterial plaques, repairing damaged tissues, or delivering personalized drug cocktails based on real-time biological feedback.
8. Blockchain for Health Data Security: Immutable Records and Patient Privacy

Blockchain technology is emerging as a transformative solution for healthcare data management, offering unprecedented security, interoperability, and patient control over medical information in an era of increasing digitization and cyber threats. This distributed ledger technology creates immutable, encrypted records that can securely store and share patient data across multiple healthcare providers while maintaining privacy and preventing unauthorized access or data tampering. The decentralized nature of blockchain eliminates single points of failure that make traditional healthcare databases vulnerable to cyberattacks, while cryptographic hashing ensures that any attempt to alter medical records is immediately detectable. Smart contracts built on blockchain platforms can automate healthcare processes such as insurance claims processing, clinical trial participant consent management, and pharmaceutical supply chain verification, reducing administrative costs and eliminating fraud. Patient-controlled health records enabled by blockchain technology give individuals ownership of their medical data, allowing them to grant or revoke access to specific healthcare providers while maintaining a complete, portable medical history that follows them throughout their healthcare journey. The technology is particularly valuable for clinical research, where blockchain can ensure data integrity, maintain participant privacy, and enable secure sharing of research data across institutions while complying with regulatory requirements. Pharmaceutical companies are utilizing blockchain to combat counterfeit drugs by creating transparent, traceable supply chains that verify the authenticity and proper handling of medications from manufacture to patient delivery. The integration of blockchain with Internet of Things (IoT) devices and wearable health monitors is creating secure ecosystems where patient-generated health data can be automatically recorded and verified without compromising privacy. As regulatory frameworks evolve and interoperability standards are established, blockchain technology promises to create a more secure, efficient, and patient-centric healthcare system where data flows seamlessly between providers while maintaining the highest standards of privacy and security.
9. Virtual and Augmented Reality in Medical Training: Immersive Learning Experiences

Virtual and augmented reality technologies are revolutionizing medical education and training by providing immersive, risk-free environments where healthcare professionals can practice complex procedures, explore human anatomy, and develop clinical skills without putting patients at risk. These technologies create highly realistic simulations that allow medical students and practicing physicians to repeatedly practice surgical procedures, emergency responses, and diagnostic techniques until they achieve mastery, significantly improving learning outcomes and patient safety. Virtual reality surgical simulators provide haptic feedback that replicates the tactile sensations of real surgery, enabling trainees to develop muscle memory and procedural confidence before operating on actual patients, while augmented reality systems can overlay digital information onto real-world environments to guide procedures and provide real-time assistance. Medical schools are incorporating VR anatomy lessons that allow students to explore three-dimensional human body structures from any angle, dissect virtual cadavers, and understand complex physiological processes through interactive visualizations that surpass traditional textbook learning. The technology is particularly valuable for training in rare or high-risk procedures where opportunities for hands-on experience are limited, enabling healthcare professionals to maintain and develop skills that might otherwise atrophy due to lack of practice. Emergency medicine training has been transformed by VR simulations that can recreate crisis scenarios with perfect reproducibility, allowing teams to practice coordination and decision-making under pressure while analyzing performance for continuous improvement. Augmented reality is advancing surgical practice by enabling surgeons to visualize internal structures, surgical plans, and critical information directly within their field of view during procedures, improving precision and reducing operative time. As these technologies become more sophisticated and affordable, they promise to democratize access to high-quality medical training globally, enabling healthcare professionals in underserved areas to receive world-class education and maintain cutting-edge skills through immersive virtual experiences.
10. Internet of Medical Things (IoMT): Connected Healthcare Ecosystems

The Internet of Medical Things represents a paradigm shift toward interconnected healthcare ecosystems where medical devices, sensors, and systems communicate seamlessly to create comprehensive, real-time pictures of patient health and healthcare operations. This network of connected medical devices includes everything from smart pill bottles that track medication adherence to sophisticated monitoring systems that continuously assess patient vital signs and automatically alert healthcare providers to concerning changes. IoMT devices generate vast amounts of data that, when analyzed using artificial intelligence and machine learning algorithms, can identify patterns and trends that enable predictive healthcare interventions and personalized treatment optimization. Smart hospitals are leveraging IoMT infrastructure to optimize operations, track equipment utilization, monitor environmental conditions, and ensure efficient resource allocation while improving patient safety through automated alerts and workflow optimization. Remote patient monitoring through IoMT devices is enabling healthcare providers to manage chronic diseases more effectively by providing continuous visibility into patient status, medication compliance, and symptom progression, reducing the need for frequent clinic visits while improving health outcomes. The integration of IoMT with electronic health records creates comprehensive digital health profiles that follow patients across different healthcare settings, ensuring continuity of care and enabling more informed clinical decision-making. Wearable IoMT devices are empowering patients to take active roles in their health management by providing real-time feedback on their physiological status, activity levels, and treatment adherence, fostering better health behaviors and improved self-care. As 5G networks expand and edge computing capabilities improve, IoMT systems will become more responsive and capable of processing complex data locally, enabling real-time clinical decision support and reducing latency in critical care situations. The future of IoMT promises even more sophisticated applications, including smart contact lenses that monitor intraocular pressure, implantable sensors that track organ function, and environmental monitoring systems that can predict and prevent disease outbreaks.
11. Digital Therapeutics: Software as Medicine

Digital therapeutics represent a groundbreaking category of evidence-based therapeutic interventions delivered through software programs, mobile applications, and digital platforms that are clinically validated to treat, manage, or prevent medical conditions. Unlike traditional health apps, digital therapeutics undergo rigorous clinical testing and regulatory approval processes similar to pharmaceutical drugs, ensuring their safety and efficacy for specific medical conditions. These software-based interventions can deliver cognitive behavioral therapy for mental health conditions, provide personalized rehabilitation programs for stroke recovery, or offer behavior modification programs for substance abuse treatment, often with outcomes comparable to or better than traditional therapeutic approaches. The FDA







