9 Wild Discoveries About the Microbes Living on Your Skin
Your skin is far more than a simple protective barrier – it's a thriving metropolis teeming with trillions of microscopic residents that form one of the most complex ecosystems on Earth. This invisible universe, known as the skin microbiome, harbors an estimated 1,000 different species of bacteria, fungi, viruses, and other microorganisms that have evolved alongside humans for millennia. Recent advances in DNA sequencing technology and microbiological research have revolutionized our understanding of these tiny inhabitants, revealing that they play crucial roles in everything from immune system function to wound healing and even mental health. Far from being mere hitchhikers, these microbes actively participate in maintaining skin health, fighting off pathogens, and communicating with our bodies in ways scientists are only beginning to comprehend. The discoveries emerging from cutting-edge research are not only reshaping dermatology and medicine but also challenging our fundamental understanding of what it means to be human. As we delve into nine remarkable findings about your skin's microbial community, prepare to see your body – and yourself – in an entirely new light.
1. Your Skin Hosts More Microbes Than There Are Stars in the Galaxy

The sheer scale of microbial life inhabiting your skin is nothing short of astronomical. Scientists estimate that the average human body hosts approximately 39 trillion microbial cells, with the vast majority residing on and within the skin's layers. To put this in perspective, this number exceeds the estimated 100-400 billion stars in our entire Milky Way galaxy by a factor of nearly 100. Your skin alone harbors roughly 1 trillion microbes per square centimeter, creating population densities that rival the most crowded cities on Earth. These microscopic communities are so densely packed that if you could shrink down to bacterial size, navigating your skin's surface would be like moving through a bustling metropolis where every available space is occupied. Recent metagenomic studies have revealed that different regions of your skin host distinct microbial neighborhoods – your oily T-zone supports different species than your dry elbows, and your feet harbor communities unlike those on your hands. This microbial census becomes even more remarkable when you consider that these populations are in constant flux, with some bacteria dividing every 20 minutes while others remain dormant for extended periods, creating a dynamic ecosystem that's perpetually evolving and adapting to your body's changing conditions.
2. Each Body Part Has Its Own Unique Microbial Fingerprint

Just as every person has unique fingerprints, each region of your body maintains its own distinct microbial signature that's as individual as your DNA. The Human Microbiome Project, a landmark scientific initiative, mapped these microbial neighborhoods and discovered that the bacterial communities on your forearm are as different from those behind your ears as the wildlife in a rainforest differs from that in a desert. Your sebaceous (oily) areas, such as your face and upper chest, are dominated by Propionibacterium species that thrive in lipid-rich environments, while your moist areas like armpits and groin favor Corynebacterium and Staphylococcus species that excel in humid conditions. Dry areas such as your forearms and legs host entirely different communities, primarily Streptococcus and Flavobacterium species adapted to lower moisture levels. What's even more fascinating is that these microbial fingerprints are so stable and unique that forensic scientists are exploring their potential use in criminal investigations. Research has shown that the microbial communities you leave on objects you touch can persist for weeks and potentially identify you with greater accuracy than traditional fingerprinting methods. This microbial individuality is shaped by factors including genetics, age, diet, lifestyle, geographic location, and even the pets you live with, creating a personalized ecosystem that's uniquely yours.
3. Your Skin Microbes Act as a Living Shield Against Dangerous Pathogens
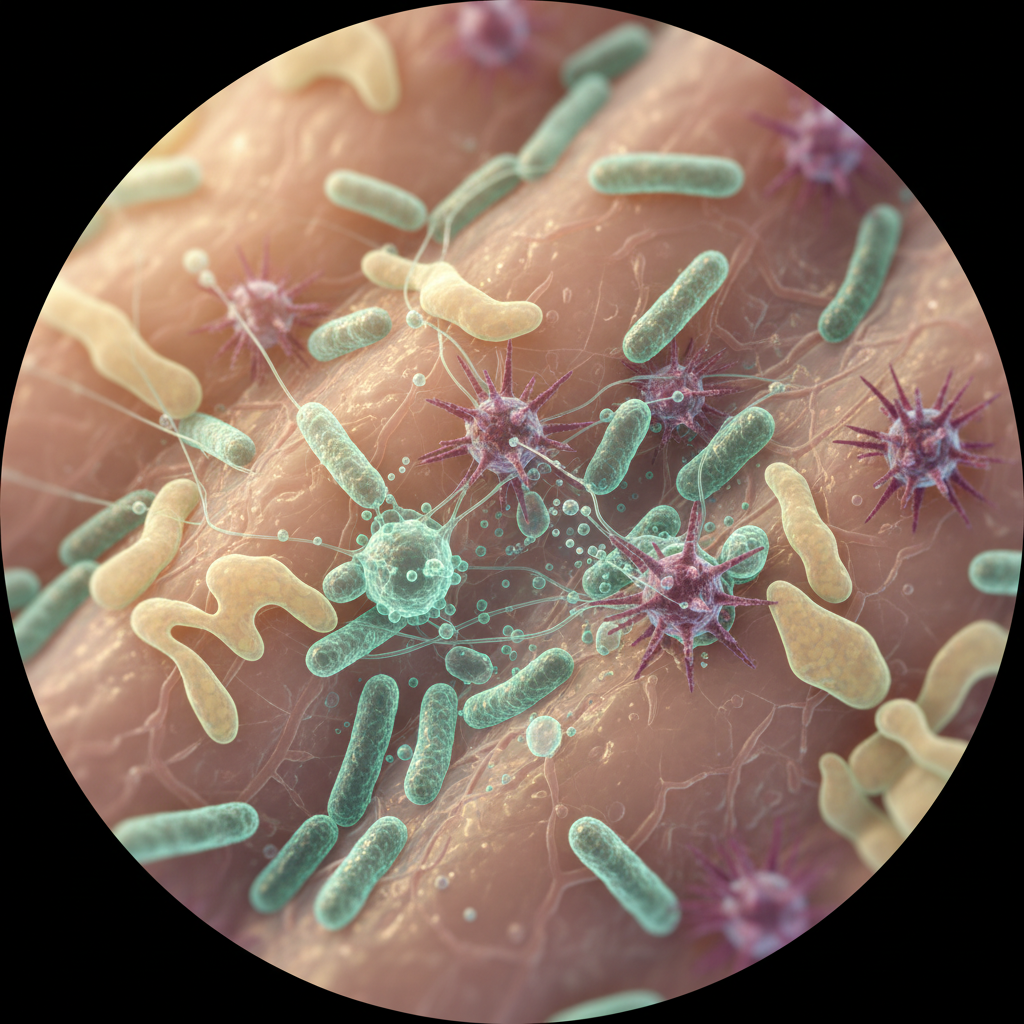
Your skin's microbial residents function as a sophisticated biological security system, actively defending you against harmful invaders through multiple ingenious mechanisms. These beneficial microbes, known as commensals, engage in what scientists call "competitive exclusion," essentially crowding out dangerous pathogens by occupying prime real estate on your skin and consuming available nutrients. Staphylococcus epidermidis, one of your skin's most abundant residents, produces antimicrobial peptides and bacteriocins that specifically target harmful bacteria like Staphylococcus aureus, including antibiotic-resistant strains like MRSA. Some skin bacteria produce natural antibiotics that are so effective that pharmaceutical companies are studying them for drug development. Research has revealed that people with diverse, healthy skin microbiomes are significantly less susceptible to skin infections, allergic reactions, and inflammatory conditions. Your microbial defenders also maintain your skin's optimal pH levels, typically around 5.5, creating an acidic environment that's hostile to many pathogens while remaining comfortable for beneficial species. Additionally, these microbes stimulate your immune system in precisely calibrated ways, training your body's defenses to recognize threats while avoiding overreactions that could lead to autoimmune conditions. When this microbial shield is disrupted by factors like overuse of antibacterial products or certain medications, your skin becomes vulnerable to colonization by opportunistic pathogens, often resulting in infections or inflammatory conditions that can be difficult to treat.
4. Skin Bacteria Produce Compounds That Influence Your Body Odor and Mood

The relationship between your skin microbes and your personal scent is far more complex and influential than most people realize, extending beyond simple body odor to potentially affect your emotions and social interactions. Different bacterial species metabolize the proteins and lipids in your sweat into distinct aromatic compounds, creating your unique olfactory signature. Corynebacterium species in your armpits break down amino acids into compounds like 3-methyl-2-hexenoic acid, which contributes to the characteristic "musky" smell, while Staphylococcus hominis produces thioalcohols that create more pungent odors. Remarkably, recent research has discovered that some skin bacteria produce neurotransmitter-like compounds that can influence mood and behavior. Certain Staphylococcus species have been found to produce gamma-aminobutyric acid (GABA), a neurotransmitter associated with relaxation and reduced anxiety, while others generate serotonin precursors that may affect emotional well-being. The skin-brain connection appears to operate through multiple pathways, including the release of volatile organic compounds that can be detected by olfactory receptors and potentially influence the limbic system. Studies have shown that people with certain microbial profiles report different stress levels and mood states, suggesting that your skin's bacterial community might be subtly influencing your mental health. This discovery has opened new avenues for research into "psychobiotic" skincare products that could potentially support both skin health and emotional well-being through targeted microbial modulation.
5. Your Skin Microbiome Changes Dramatically Throughout Your Lifetime
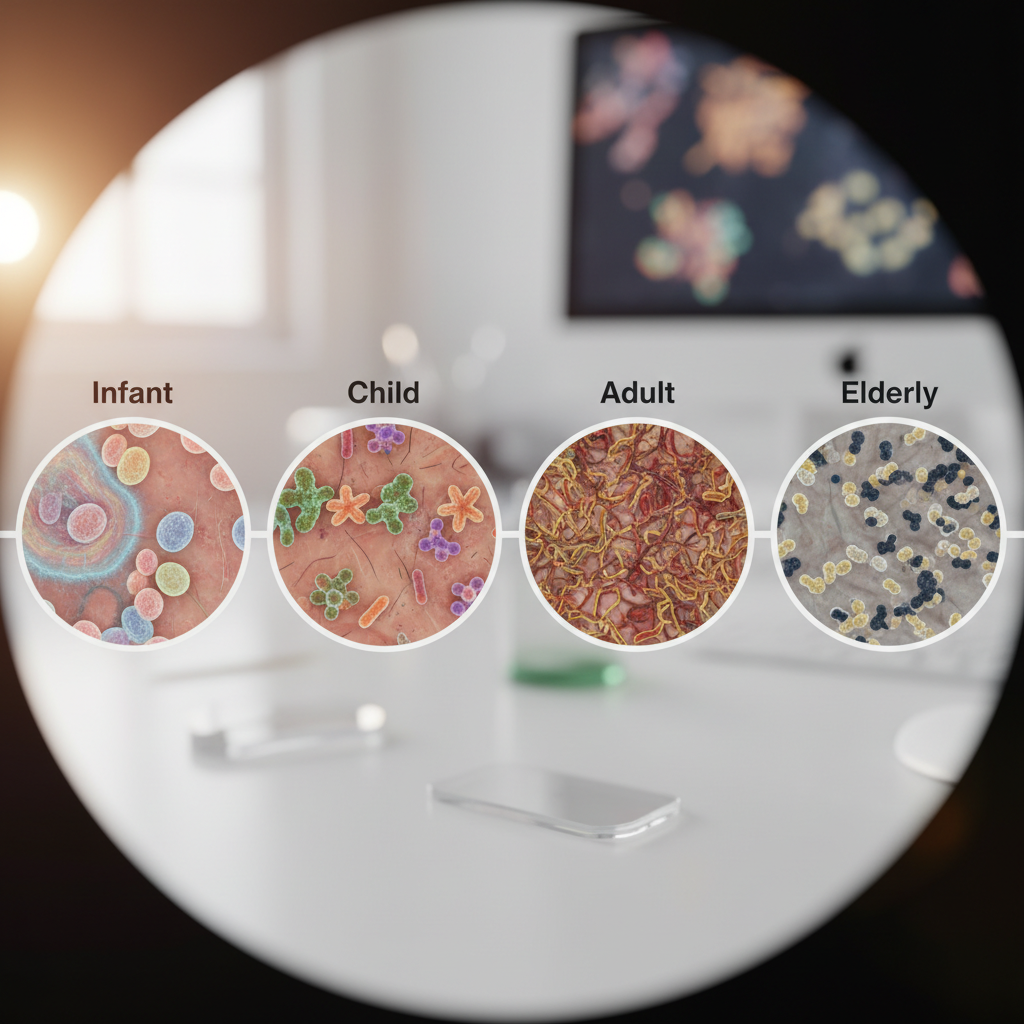
The microbial landscape of your skin undergoes remarkable transformations throughout your life, creating distinct chapters in your personal microbiome story that reflect major biological and environmental changes. Newborn babies emerge from the sterile environment of the womb with virtually no skin microbes, but within hours of birth, they begin acquiring their first microbial colonizers from their mother's skin, the birth canal, and the surrounding environment. During the first year of life, an infant's skin microbiome develops rapidly, influenced by factors such as delivery method (vaginal vs. cesarean), feeding type (breast milk vs. formula), and early environmental exposures. The microbial community reaches a relatively stable state during childhood, dominated by species well-suited to the unique conditions of young skin. However, puberty brings dramatic changes as hormonal fluctuations alter skin chemistry, increasing oil production and creating new ecological niches that favor different bacterial species – explaining why acne often emerges during adolescence. Adult skin maintains relatively stable microbial communities for several decades, but aging introduces new changes as skin becomes thinner, drier, and less acidic, favoring different microbial populations. Elderly individuals often show decreased microbial diversity and altered community structures that may contribute to increased susceptibility to skin infections and slower wound healing. Environmental factors throughout life, including geographic relocations, dietary changes, medication use, and lifestyle modifications, continuously shape these microbial communities, creating a dynamic biological record of your life experiences written in bacterial DNA.
6. Disrupting Your Skin Microbiome Can Lead to Serious Health Consequences
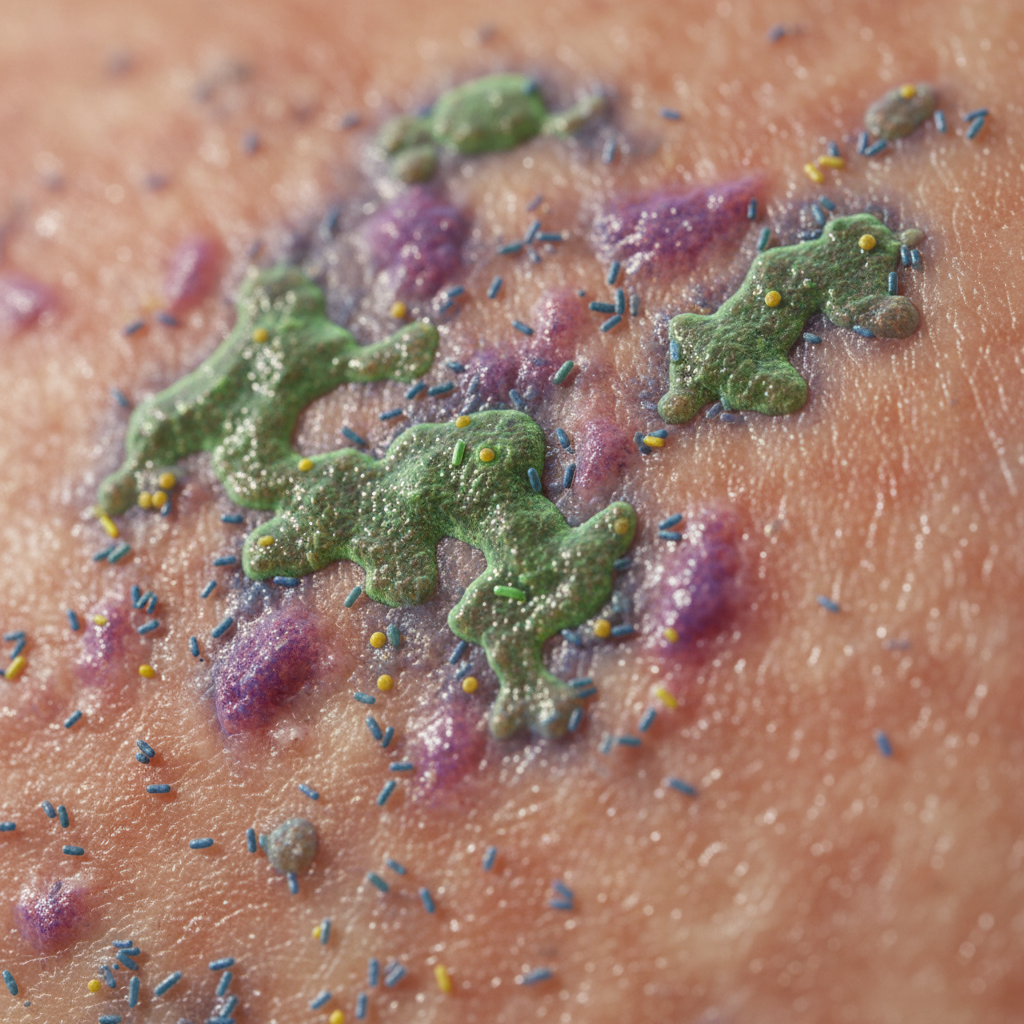
The delicate balance of your skin's microbial ecosystem can be easily disrupted, leading to a cascade of health problems that extend far beyond simple skin irritation. This disruption, known as dysbiosis, occurs when the normal microbial community structure is altered, often resulting in the overgrowth of potentially harmful species or the loss of beneficial ones. Overuse of antibacterial soaps, hand sanitizers, and topical antibiotics can indiscriminately kill both harmful and beneficial bacteria, creating ecological voids that opportunistic pathogens quickly fill. Research has linked skin microbiome disruption to a wide range of conditions, including eczema, psoriasis, acne, and even more serious systemic infections. Studies have shown that children who grow up in overly sanitized environments often develop compromised skin microbiomes and higher rates of allergies and autoimmune conditions, supporting the "hygiene hypothesis" that some microbial exposure is necessary for proper immune system development. Hospital-acquired infections often begin when medical procedures or antimicrobial treatments disrupt patients' protective skin microbiomes, allowing drug-resistant bacteria to establish footholds. The consequences can be particularly severe for immunocompromised individuals, elderly patients, or those with chronic conditions. Emerging research suggests that skin microbiome disruption may also affect wound healing, skin barrier function, and even influence systemic inflammation levels. Recovery from severe dysbiosis can take weeks or months, during which the skin remains vulnerable to colonization by pathogens and may experience persistent inflammation, highlighting the importance of maintaining microbial balance through thoughtful skincare practices.
7. Skin Microbes Communicate With Each Other Through Chemical Signals

Your skin's microbial residents engage in sophisticated chemical communication networks that rival the complexity of human social systems, coordinating their activities through a process called quorum sensing. This bacterial "language" involves the production and detection of signaling molecules that allow microbes to assess population density, coordinate group behaviors, and respond collectively to environmental changes. When bacterial populations reach certain thresholds, they release specific chemical signals that trigger coordinated responses such as biofilm formation, toxin production, or metabolic shifts that affect the entire microbial community. Staphylococcus epidermidis, for example, produces autoinducing peptides that help coordinate the formation of protective biofilms and regulate the production of antimicrobial compounds. These communication networks create a form of bacterial democracy where individual microbes vote through chemical signals to determine community-wide decisions. Research has revealed that disrupting these communication pathways can be an effective strategy for treating bacterial infections without relying on traditional antibiotics, which often lead to resistance. Some skin bacteria also engage in cross-species communication, sending chemical messages that can influence the behavior of entirely different microbial species, fungi, and even human skin cells. Scientists have discovered that certain bacterial signals can trigger human cells to increase production of antimicrobial peptides or modify immune responses, demonstrating that the communication extends beyond the microbial world to include direct dialogue with your body's own cells. Understanding these communication networks is opening new possibilities for developing targeted therapies that could modulate skin health by influencing bacterial behavior rather than simply killing microbes.
8. Your Diet and Lifestyle Directly Shape Your Skin's Microbial Community

The foods you eat, the places you live, and the lifestyle choices you make have profound and measurable effects on the microbial communities inhabiting your skin, creating a direct link between your daily habits and your skin's health. Research has shown that dietary changes can alter skin microbiome composition within just a few days, with high-sugar diets promoting the growth of certain bacterial species while fiber-rich diets support others. People who consume fermented foods like yogurt, kefir, and kimchi often have more diverse skin microbiomes, possibly due to the introduction of beneficial bacteria through the gut-skin axis. Geographic location plays a crucial role, with studies revealing that people living in urban environments have markedly different skin microbiomes compared to those in rural areas, likely due to differences in air quality, water composition, and exposure to environmental microbes. Your exercise habits also influence your skin's microbial landscape – regular physical activity promotes beneficial bacterial diversity, while sedentary lifestyles are associated with less diverse and potentially less healthy microbial communities. Sleep patterns, stress levels, and even the materials of your clothing and bedding can impact your skin's bacterial residents. People who work in healthcare settings, food service, or agriculture develop occupational microbial signatures that reflect their professional environments. Surprisingly, pet ownership significantly influences human skin microbiomes, with dog owners sharing certain bacterial species with their pets. Climate and seasonal changes also drive microbial shifts, with winter's dry conditions favoring different species than summer's heat and humidity. These findings suggest that optimizing skin health might require a holistic approach that considers not just topical treatments but entire lifestyle patterns.
9. Scientists Are Developing Probiotic Skincare to Enhance Your Skin's Microbiome

The growing understanding of skin microbiome importance has sparked a revolution in skincare science, leading to the development of sophisticated probiotic and prebiotic products designed to support and enhance your skin's natural microbial communities. Unlike traditional skincare that often focuses on eliminating bacteria, these innovative approaches work with your skin's ecosystem to promote beneficial microbial growth and restore healthy balance. Live probiotic skincare products contain carefully selected strains of beneficial bacteria that can colonize the skin and compete with harmful pathogens, while prebiotic formulations provide nutrients that selectively feed beneficial microbes already present on your skin. Companies are developing strain-specific treatments targeting particular skin conditions – for example, Lactobacillus plantarum has shown promise for treating acne by producing antimicrobial compounds that specifically target Propionibacterium acnes. Postbiotic skincare represents another frontier, utilizing beneficial compounds produced by bacteria, such as peptides, enzymes, and metabolites, without including live microorganisms. Clinical trials have demonstrated that microbiome-targeted treatments can effectively address conditions ranging from eczema and rosacea to premature aging and wound healing. Some researchers are exploring personalized microbiome therapy, where an individual's skin microbiome is analyzed to create customized probiotic treatments tailored to their specific microbial profile and skin needs. The challenge lies in ensuring that beneficial bacteria can survive the journey from laboratory to skin while remaining stable in cosmetic formulations. Advanced encapsulation technologies and innovative delivery systems are being developed to protect live probiotics and ensure they reach their target locations on the skin in viable form, potentially transforming how we approach skin health and beauty.
10. The Future of Medicine May Involve Microbiome Transplants and Bacterial Therapies

The frontier of microbiome medicine is rapidly advancing toward revolutionary treatments that could fundamentally change how we approach skin health, infectious diseases, and even systemic medical conditions. Researchers are developing skin microbiome transplant procedures, similar to fecal microbiota transplantation used for gut health, where healthy microbial communities from donors are transferred to patients with compromised skin microbiomes. Early clinical trials have shown promising results for treating chronic skin conditions like severe eczema and recurrent infections that haven't responded to conventional therapies. Scientists are also engineering beneficial bacteria to serve as living therapeutics, genetically modifying skin commensals to produce specific therapeutic compounds directly on the skin's surface. These "designer microbes" could potentially deliver medications continuously, monitor health conditions through biosensing capabilities, or even detect and neutralize environmental toxins before they penetrate the skin. The concept of "bacterial bandages" is being explored, where beneficial microbes are incorporated into wound dressings to accelerate healing and prevent infections. Researchers envision a future where routine microbiome analysis becomes as common as blood tests, allowing doctors to diagnose conditions, monitor treatment progress, and predict health risks based on microbial signatures. The potential extends beyond dermatology – skin microbiome profiles may serve as biomarkers for systemic diseases, mental health conditions, and even aging processes. As our understanding deepens, we may discover that optimizing our skin's microbial communities could influence everything from immune function to longevity, making microbiome management a cornerstone of preventive medicine and personalized healthcare in the decades to come.







