9 Recent Findings About How Stress Physically Damages the Body
In our increasingly fast-paced world, stress has evolved from an occasional challenge into a chronic companion for millions of people worldwide. While we've long understood that stress affects our mental well-being, groundbreaking research over the past decade has revealed the profound and often irreversible physical damage that chronic stress inflicts on our bodies. From cellular aging to organ dysfunction, the physiological consequences of sustained stress response extend far beyond the temporary discomfort we might feel during challenging moments. Recent scientific investigations have uncovered nine particularly alarming ways that stress literally rewrites our biology, accelerating disease processes, compromising immune function, and fundamentally altering how our bodies operate at the most basic levels. These findings represent a paradigm shift in our understanding of stress-related health consequences, moving beyond psychological symptoms to reveal a complex web of physical deterioration that affects every major body system. The implications of this research are staggering, suggesting that chronic stress may be one of the most significant public health threats of our time, silently damaging our bodies in ways that were previously unimaginable.
1. Cellular Aging Acceleration Through Telomere Shortening

One of the most startling discoveries in stress research involves the direct impact of chronic stress on cellular aging through telomere degradation. Telomeres, the protective caps at the ends of chromosomes, naturally shorten as we age, but recent studies have shown that chronic stress dramatically accelerates this process, effectively aging our cells at a molecular level. Research published in leading journals has demonstrated that individuals experiencing prolonged stress show telomere lengths equivalent to those found in people decades older, with some studies indicating that chronic stress can add up to 17 years to biological age. The mechanism behind this acceleration involves elevated cortisol levels, which directly interfere with telomerase, the enzyme responsible for maintaining telomere length. When stress hormones remain chronically elevated, they create a toxic cellular environment that not only shortens existing telomeres but also impairs the body's ability to repair and maintain these crucial protective structures. This cellular aging process has far-reaching consequences, as shortened telomeres are associated with increased risk of cancer, cardiovascular disease, cognitive decline, and premature death. The research suggests that stress-induced telomere shortening may be one of the primary pathways through which psychological stress translates into physical disease and accelerated aging.
2. Immune System Suppression and Inflammatory Response Dysfunction

Recent immunological research has revealed that chronic stress fundamentally rewires the immune system, creating a state of persistent inflammation while simultaneously suppressing the body's ability to fight infections and heal wounds. Studies using advanced biomarker analysis have shown that individuals under chronic stress exhibit elevated levels of inflammatory cytokines, particularly interleukin-6 and tumor necrosis factor-alpha, which remain persistently high even during periods of apparent calm. This chronic inflammatory state, termed "inflammaging" by researchers, accelerates the development of autoimmune disorders, increases susceptibility to infections, and promotes the growth of cancer cells. Simultaneously, stress hormones suppress the production and function of key immune cells, including natural killer cells and T-lymphocytes, which are crucial for identifying and eliminating threats to the body. The paradox of heightened inflammation coupled with immune suppression creates a perfect storm for disease development. Recent longitudinal studies have demonstrated that individuals with chronic stress show delayed wound healing, increased frequency of viral infections, reduced vaccine effectiveness, and higher rates of autoimmune disease onset. The research indicates that stress-induced immune dysfunction may persist for months or even years after the initial stressor has been removed, suggesting that the damage to immune function represents a long-term consequence rather than a temporary adaptation.
3. Cardiovascular System Damage and Heart Disease Acceleration
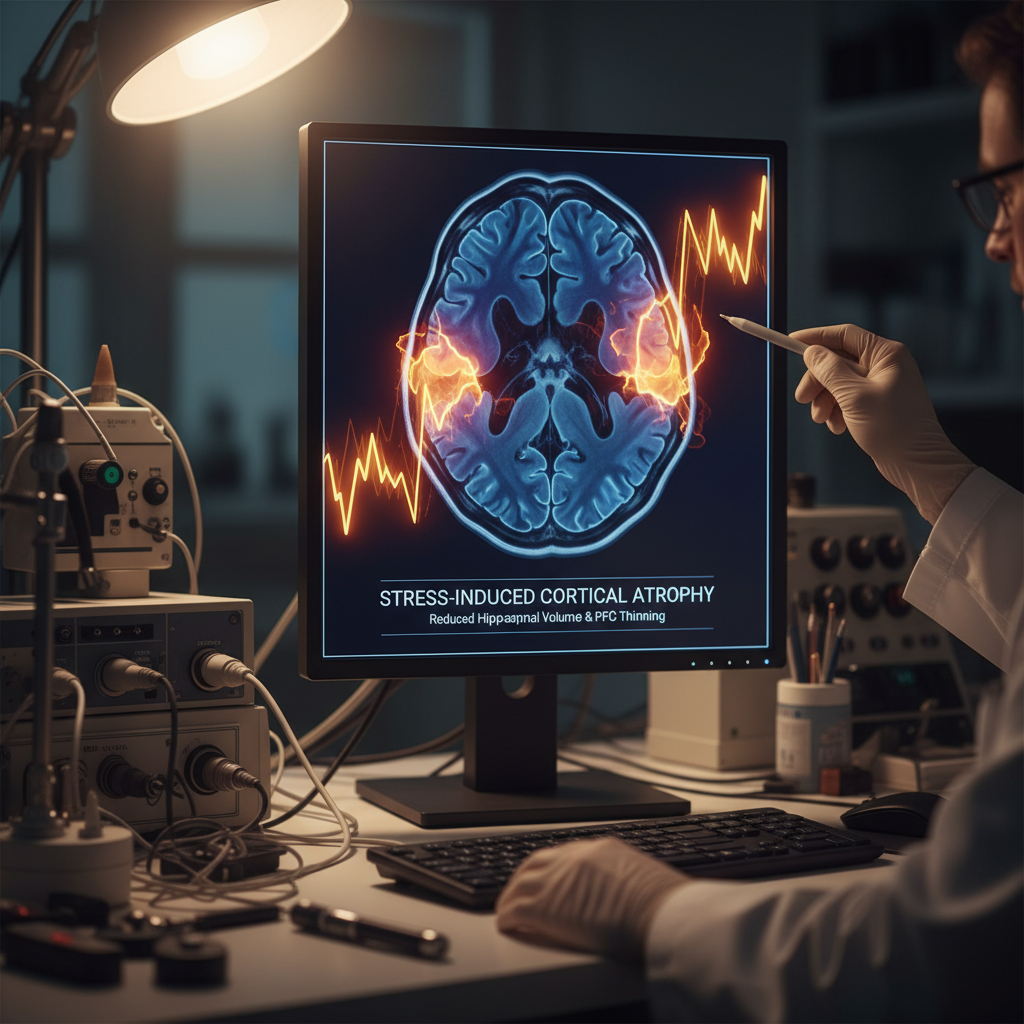
Groundbreaking cardiovascular research has unveiled the devastating impact of chronic stress on heart health, revealing mechanisms that extend far beyond the traditional understanding of stress-related heart problems. Advanced imaging studies have shown that chronic stress directly damages the arterial walls, promoting atherosclerosis through multiple pathways including increased blood pressure, elevated cholesterol production, and enhanced platelet aggregation. Recent research has identified that stress hormones, particularly cortisol and adrenaline, cause microscopic tears in arterial walls, which become sites for plaque accumulation and eventual blockage. Additionally, chronic stress alters heart rhythm variability, reducing the heart's ability to adapt to changing demands and increasing the risk of sudden cardiac events. Studies utilizing continuous monitoring technology have demonstrated that individuals under chronic stress show persistent elevation in heart rate and blood pressure, even during sleep, indicating that the cardiovascular system never truly recovers from stress activation. The research has also revealed that stress-induced inflammation directly contributes to the instability of arterial plaques, making them more likely to rupture and cause heart attacks or strokes. Perhaps most concerning, recent findings suggest that the cardiovascular damage from chronic stress may be largely irreversible, with stress-exposed individuals showing permanently altered cardiac function even years after stress reduction interventions.
4. Neurological Deterioration and Brain Structure Changes
Cutting-edge neuroimaging research has revealed that chronic stress literally reshapes the brain, causing structural changes that impair cognitive function and increase vulnerability to neurological disorders. Advanced MRI studies have documented that prolonged stress exposure leads to significant shrinkage in the prefrontal cortex, the brain region responsible for executive function, decision-making, and emotional regulation. Simultaneously, chronic stress causes enlargement of the amygdala, the brain's fear center, creating a state of hypervigilance and emotional reactivity that becomes increasingly difficult to control. Recent research has shown that stress hormones, particularly cortisol, are directly toxic to brain cells, causing neuronal death and preventing the formation of new neural connections. This neuroplasticity disruption has profound implications for learning, memory, and adaptation to new situations. Studies have also revealed that chronic stress accelerates the accumulation of beta-amyloid plaques and tau proteins in the brain, the hallmark pathologies of Alzheimer's disease, effectively fast-tracking the development of dementia. The research indicates that stress-induced brain changes begin within weeks of exposure and may become permanent if the stress continues for extended periods. Additionally, chronic stress disrupts the blood-brain barrier, allowing toxins and inflammatory molecules to enter brain tissue, further accelerating neurological deterioration and increasing the risk of stroke, depression, and cognitive decline.
5. Digestive System Disruption and Gut Health Compromise

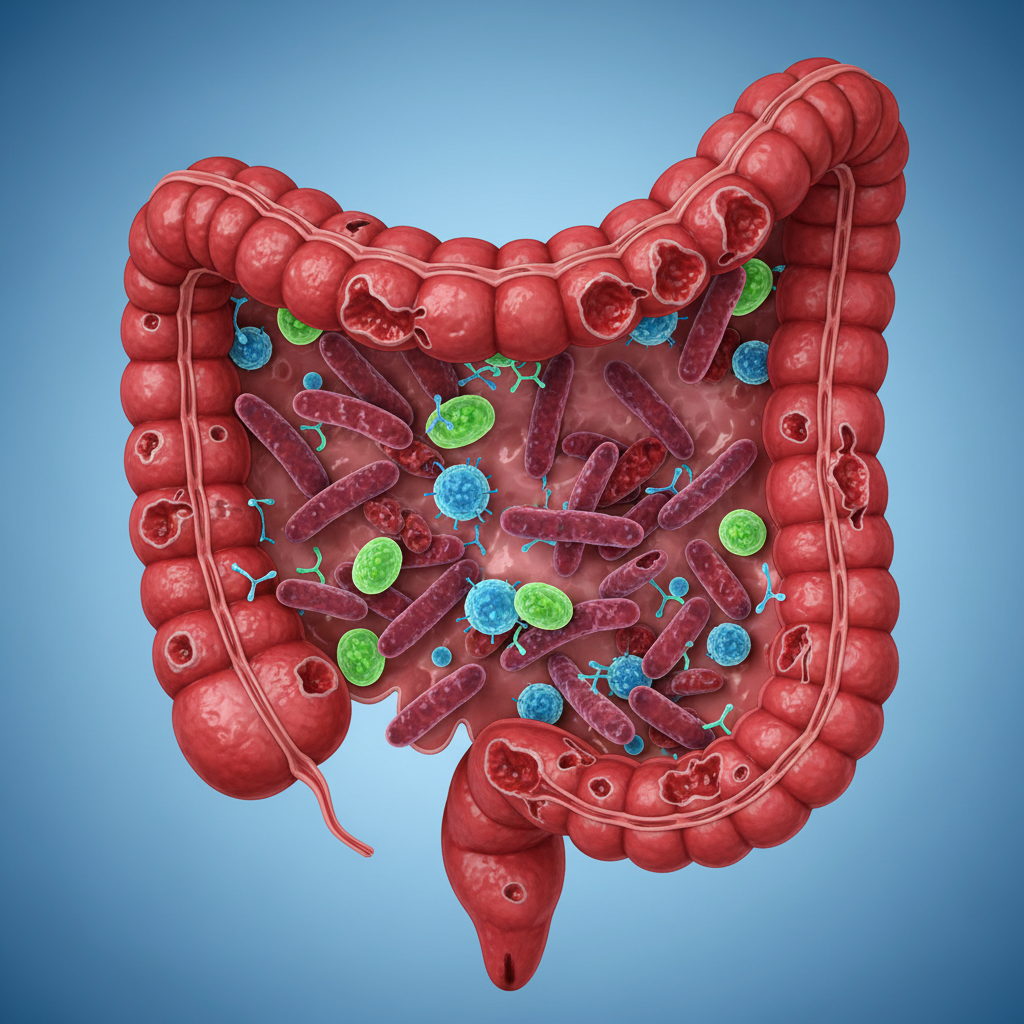
Revolutionary research in gastroenterology has uncovered the profound impact of chronic stress on digestive health, revealing a complex interplay between stress hormones and gut function that extends far beyond occasional stomach upset. Recent studies have demonstrated that chronic stress fundamentally alters the gut microbiome, reducing beneficial bacteria populations while promoting the growth of pathogenic organisms, leading to a state called dysbiosis. This microbial imbalance has far-reaching consequences, as the gut microbiome plays crucial roles in immune function, neurotransmitter production, and nutrient absorption. Advanced research has shown that stress hormones directly damage the intestinal lining, increasing intestinal permeability in a condition known as "leaky gut syndrome," which allows toxins and undigested food particles to enter the bloodstream and trigger systemic inflammation. Chronic stress also disrupts normal digestive motility, leading to conditions such as irritable bowel syndrome, gastroparesis, and increased risk of peptic ulcers. Recent findings have revealed that stress-induced changes in gut function can persist for months after the initial stressor has been removed, suggesting that digestive damage represents a long-term consequence of stress exposure. The research has also uncovered bidirectional communication between the gut and brain, known as the gut-brain axis, where stress-induced gut dysfunction further exacerbates psychological stress, creating a vicious cycle of deteriorating health.
6. Endocrine System Disruption and Hormonal Imbalances
Sophisticated endocrinological research has revealed that chronic stress creates widespread hormonal chaos throughout the body, disrupting virtually every aspect of endocrine function and leading to cascading health problems. Recent studies have shown that prolonged stress exposure dysregulates the hypothalamic-pituitary-adrenal (HPA) axis, the body's primary stress response system, leading to either excessive cortisol production or, paradoxically, cortisol depletion in cases of extreme chronic stress. This hormonal disruption has profound effects on metabolism, with chronic stress promoting insulin resistance, increasing blood sugar levels, and accelerating the development of type 2 diabetes. Advanced research has demonstrated that stress hormones interfere with thyroid function, leading to hypothyroidism and metabolic slowdown, while simultaneously disrupting reproductive hormones, causing irregular menstrual cycles, reduced fertility, and decreased libido. Recent findings have shown that chronic stress also interferes with growth hormone production, impairing tissue repair and muscle maintenance, while disrupting melatonin production, leading to sleep disorders that further exacerbate stress-related health problems. The research indicates that stress-induced hormonal imbalances create a state of metabolic dysfunction that promotes weight gain, particularly dangerous visceral fat accumulation around organs. Perhaps most concerning, studies have revealed that these hormonal disruptions can become self-perpetuating, with damaged endocrine organs becoming less responsive to regulatory signals, leading to permanent hormonal imbalances even after stress reduction.
7. Musculoskeletal System Deterioration and Chronic Pain Development
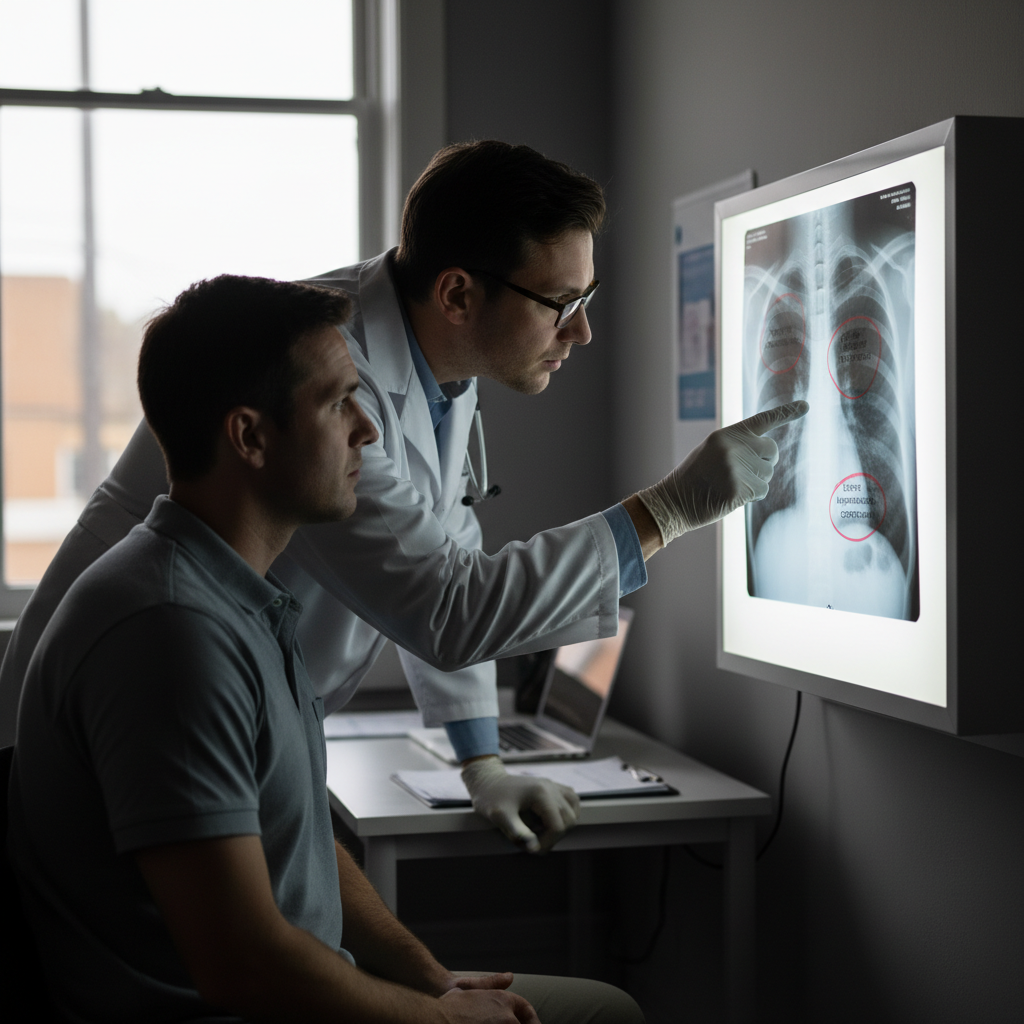
Groundbreaking research in orthopedics and pain medicine has uncovered the devastating impact of chronic stress on the musculoskeletal system, revealing mechanisms that transform temporary muscle tension into permanent structural damage and chronic pain conditions. Advanced imaging studies have shown that chronic stress leads to persistent muscle contraction and inflammation, particularly in the neck, shoulders, and back, which over time causes structural changes in muscle fibers and surrounding connective tissues. Recent research has demonstrated that stress hormones directly interfere with muscle protein synthesis while promoting protein breakdown, leading to muscle wasting and weakness despite normal activity levels. The studies have also revealed that chronic stress disrupts bone metabolism, reducing bone density and increasing fracture risk through mechanisms involving cortisol's interference with calcium absorption and bone-building cell function. Innovative pain research has shown that chronic stress actually rewires pain processing pathways in the brain and spinal cord, creating a state of central sensitization where normal sensations are perceived as painful. This neuroplastic change explains why stress-related pain conditions often persist long after the initial injury has healed. Recent findings have also demonstrated that stress-induced inflammation directly damages joint cartilage and promotes the development of arthritis, while simultaneously impairing the body's ability to repair damaged tissues. The research suggests that chronic stress may be a primary driver of many unexplained chronic pain conditions, creating a cycle where pain increases stress, which in turn amplifies pain perception and tissue damage.
8. Respiratory System Compromise and Breathing Dysfunction

Revolutionary pulmonary research has revealed that chronic stress profoundly impacts respiratory function, creating breathing difficulties that extend far beyond the temporary shortness of breath experienced during acute stress episodes. Recent studies have shown that chronic stress leads to persistent changes in breathing patterns, promoting shallow, rapid breathing that reduces oxygen efficiency and increases carbon dioxide retention, creating a state of chronic respiratory alkalosis. Advanced research has demonstrated that stress hormones cause inflammation and constriction of the airways, increasing the risk of asthma development and exacerbating existing respiratory conditions. The studies have also revealed that chronic stress impairs the function of respiratory muscles, particularly the diaphragm, leading to decreased lung capacity and increased reliance on accessory breathing muscles, which become chronically tense and painful. Recent findings have shown that stress-induced breathing dysfunction creates a cascade of physiological problems, including reduced oxygen delivery to tissues, impaired cellular metabolism, and increased fatigue. The research has also uncovered that chronic stress promotes the development of sleep-disordered breathing, including sleep apnea, which further compromises respiratory function and sleep quality. Additionally, studies have demonstrated that stress-related breathing problems can become self-perpetuating, as poor breathing patterns increase anxiety and stress levels, creating a vicious cycle of respiratory dysfunction. The implications of this research are particularly concerning given that proper breathing is fundamental to all cellular processes, suggesting that stress-induced respiratory compromise may underlie many other stress-related health problems.
9. Skin Health Degradation and Accelerated Aging

Cutting-edge dermatological research has unveiled the profound impact of chronic stress on skin health, revealing mechanisms that accelerate visible aging while compromising the skin's protective and healing functions. Recent studies have shown that chronic stress dramatically increases the production of cortisol, which breaks down collagen and elastin, the proteins responsible for skin elasticity and firmness, leading to premature wrinkles, sagging, and loss of skin tone. Advanced research has demonstrated that stress hormones also impair the skin's barrier function, reducing its ability to retain moisture and protect against environmental toxins, leading to increased sensitivity, dryness, and susceptibility to infections. The studies have revealed that chronic stress disrupts the skin's natural repair processes, significantly slowing wound healing and increasing the risk of scarring and infection. Recent findings have shown that stress-induced inflammation in the skin promotes the development of various dermatological conditions, including acne, eczema, psoriasis, and rosacea, while exacerbating existing skin problems. The research has also uncovered that chronic stress accelerates the breakdown of hyaluronic acid in the skin, leading to increased dryness and loss of volume, while simultaneously promoting the formation of advanced glycation end products (AGEs), which cause skin stiffening and yellowing. Additionally, studies have demonstrated that stress-related sleep disruption further compromises skin health by interfering with the natural overnight repair processes, leading to dull, uneven skin tone and increased signs of aging. The implications of this research extend beyond cosmetic concerns, as compromised skin barrier function can lead to increased absorption of toxins and allergens, potentially triggering systemic health problems.
10. Metabolic Disruption and Weight Management Challenges
Comprehensive metabolic research has revealed that chronic stress creates profound disruptions in the body's energy management systems, leading to weight gain, metabolic syndrome, and increased risk of diabetes through multiple interconnected pathways. Recent studies have shown that chronic stress fundamentally alters appetite regulation by disrupting the balance of hunger hormones, particularly increasing ghrelin (hunger hormone) while reducing leptin (satiety hormone), leading to increased food cravings and overeating behaviors. Advanced research has demonstrated that stress hormones, especially cortisol, promote the storage of fat in the abdominal region, creating dangerous visceral adiposity that surrounds vital organs and increases inflammation throughout the body. The studies have revealed that chronic stress also impairs glucose metabolism by promoting insulin resistance, making it increasingly difficult for cells to utilize glucose effectively and leading to elevated blood sugar levels and eventual type 2 diabetes development. Recent findings have shown that stress-induced metabolic dysfunction extends to lipid metabolism, increasing the production of triglycerides and LDL cholesterol while reducing beneficial HDL cholesterol, creating a lipid profile that promotes cardiovascular disease. The research has also uncovered that chronic stress disrupts circadian rhythms, which are crucial for proper metabolic function, leading to altered eating patterns, disrupted sleep, and further metabolic dysfunction. Additionally, studies have demonstrated that stress-related changes in gut bacteria composition directly impact metabolism, with certain stress-induced bacterial populations promoting weight gain and metabolic dysfunction. Perhaps most concerning, the research indicates that stress-induced metabolic changes can become self-perpetuating, as metabolic dysfunction increases physical stress on the body, creating a cycle of deteriorating metabolic health that becomes increasingly difficult to break without comprehensive intervention addressing both stress management and metabolic restoration.







